When it comes to sports, staying healthy is just as important as playing hard. A serious injury can knock you out of the game for weeks—or even months—whether you’re a pro athlete or simply enjoying weekend competition. The good news is that many common injuries can be prevented with a few smart adjustments to your training and lifestyle.
Exercise is good for the body and with the proper precautions, sports injuries can often be prevented. The quality of protective equipment – padding, helmets, shoes, mouth guards – has helped to improve safety in sports. But, you can still be susceptible to injury. Always contact your healthcare provider before starting any type of physical activity, especially vigorous types of exercises or sports.
Causes of sports injuries may include:
- Improper or poor training practices
- Wearing improper sporting gear
- Being in poor health condition
- Improper warm-up or stretching practices before a sporting event or exercise
Common sports injuries include:
- Sprains and strains
- Joint injuries (knee)
- Muscle injuries
- Dislocations
- Fractures
- Achilles tendon injuries
- Pain along the shin bone
How can I prevent a sports injury?
The following are some basic steps to prevent a sports injury:
- Develop a fitness plan that includes cardiovascular exercise, strength training, and flexibility. This will help decrease your chance of injury.
- Alternate exercising different muscle groups and exercise every other day.
- Cooldown properly after exercise or sports. It should take 2 times as long as your warm-ups.
- Stay hydrated. Drink water to prevent dehydration, heat exhaustion, and heatstroke.
- Stretching exercises can improve the ability of muscles to contract and perform, reducing the risk of injury. Each stretch should start slowly until you reach a point of muscle tension. Stretching should not be painful. Aim to hold each stretch for up to 20 seconds.
- Use the right equipment or gear and wear shoes that provide support and that may correct certain foot problems that can lead to injury.
- Learn the right techniques to play your sport.
- Rest when tired, Avoid exercise when you are tired or in pain.
- Always take your time during strength training and go through the full range of motion with each repetition.
- If you do sustain a sports injury, make sure you participate in adequate rehabilitation before resuming strenuous activity.

At Rausch Physical Therapy, we go beyond treating injuries—we help athletes of every level stay in peak condition so they can keep doing what they love. Our team develops personalized prevention plans that focus on strengthening weak points, improving flexibility, correcting movement patterns, and reducing risk factors unique to your sport. This proactive approach keeps you on the field, the court, or the track longer and performing at your best.
👉 Don’t wait until an injury sidelines you. Call us today at 949-276-5401 to schedule your sports injury prevention session. And don’t forget we have RX Massage and Stretch Fix to support your best health! For daily insights and performance tips, follow us on Instagram @rauschpt.
Reference: [Read more here about prevention strategies from Johns Hopkins Medicine.]








 Struggling with discomfort or limited movement due to tight hips? Don’t let it hold you back! Call our physical therapy center today at 949-276-5401 and take the first step towards a more comfortable, active life. Our comprehensive approach helps you heal faster, move better, and stay stronger for the long run.
Struggling with discomfort or limited movement due to tight hips? Don’t let it hold you back! Call our physical therapy center today at 949-276-5401 and take the first step towards a more comfortable, active life. Our comprehensive approach helps you heal faster, move better, and stay stronger for the long run. 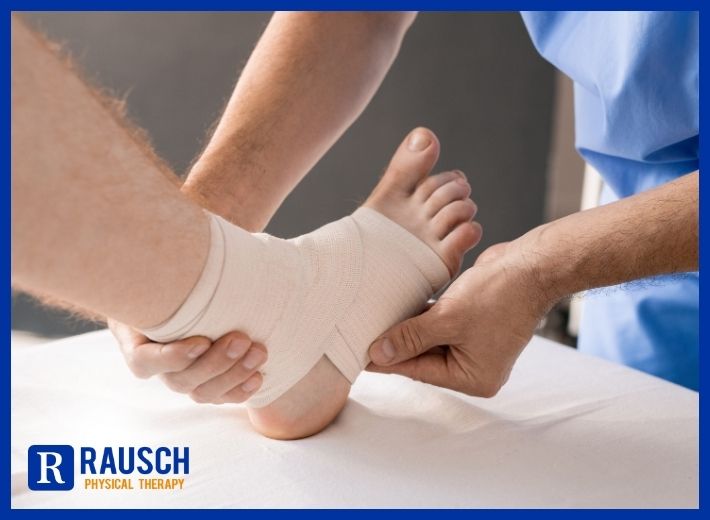

 Management and Treatment
Management and Treatment



 Light Exercise
Light Exercise Preventing DOMS
Preventing DOMS


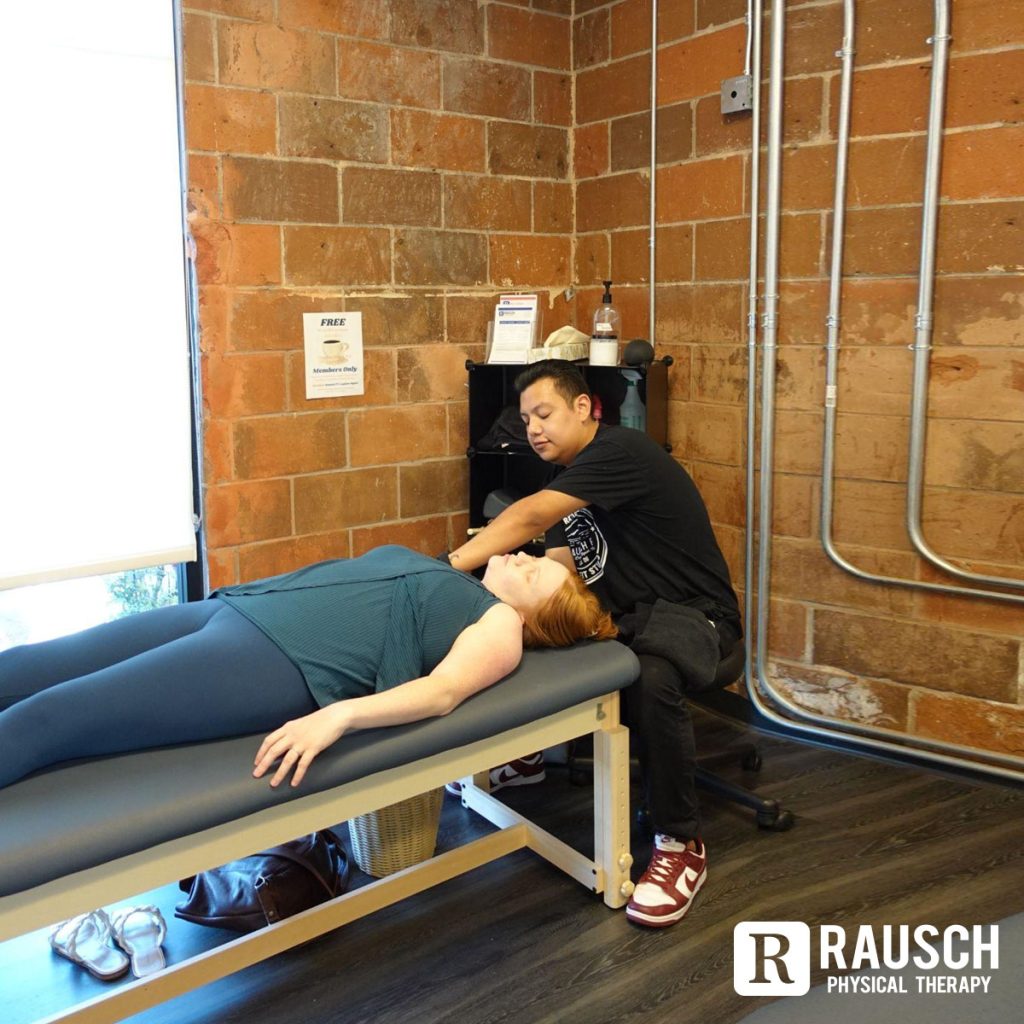




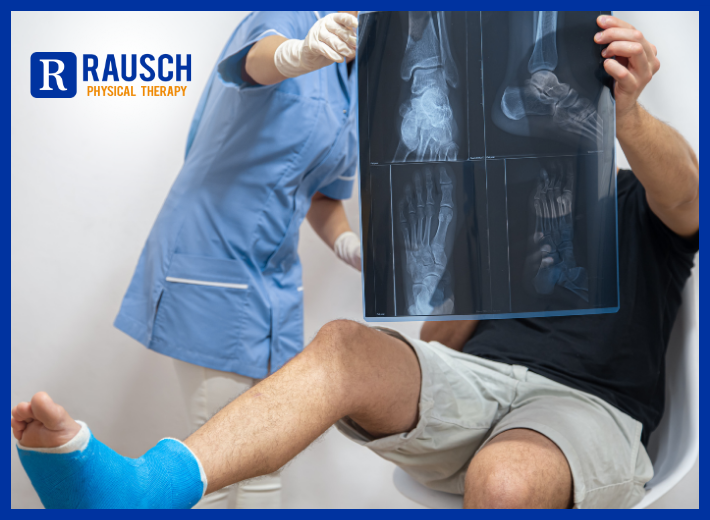
 If your doctor suggests something to help you, like a cane, walker, or reaching tool, use it. While it might seem that it keeps you from moving the way you want to, it can keep you safe and help you hurt less. And it can make it easier for you to move. That’s key: The more active you are, the better it is for your bones and overall health.
If your doctor suggests something to help you, like a cane, walker, or reaching tool, use it. While it might seem that it keeps you from moving the way you want to, it can keep you safe and help you hurt less. And it can make it easier for you to move. That’s key: The more active you are, the better it is for your bones and overall health. Take control of your recovery and get back to doing what you love. Our personalized physical therapists can provide expert advice and practical tips to help you heal and regain your strength faster. Call us today at 949-276-5401. For more tips, follow us on
Take control of your recovery and get back to doing what you love. Our personalized physical therapists can provide expert advice and practical tips to help you heal and regain your strength faster. Call us today at 949-276-5401. For more tips, follow us on 
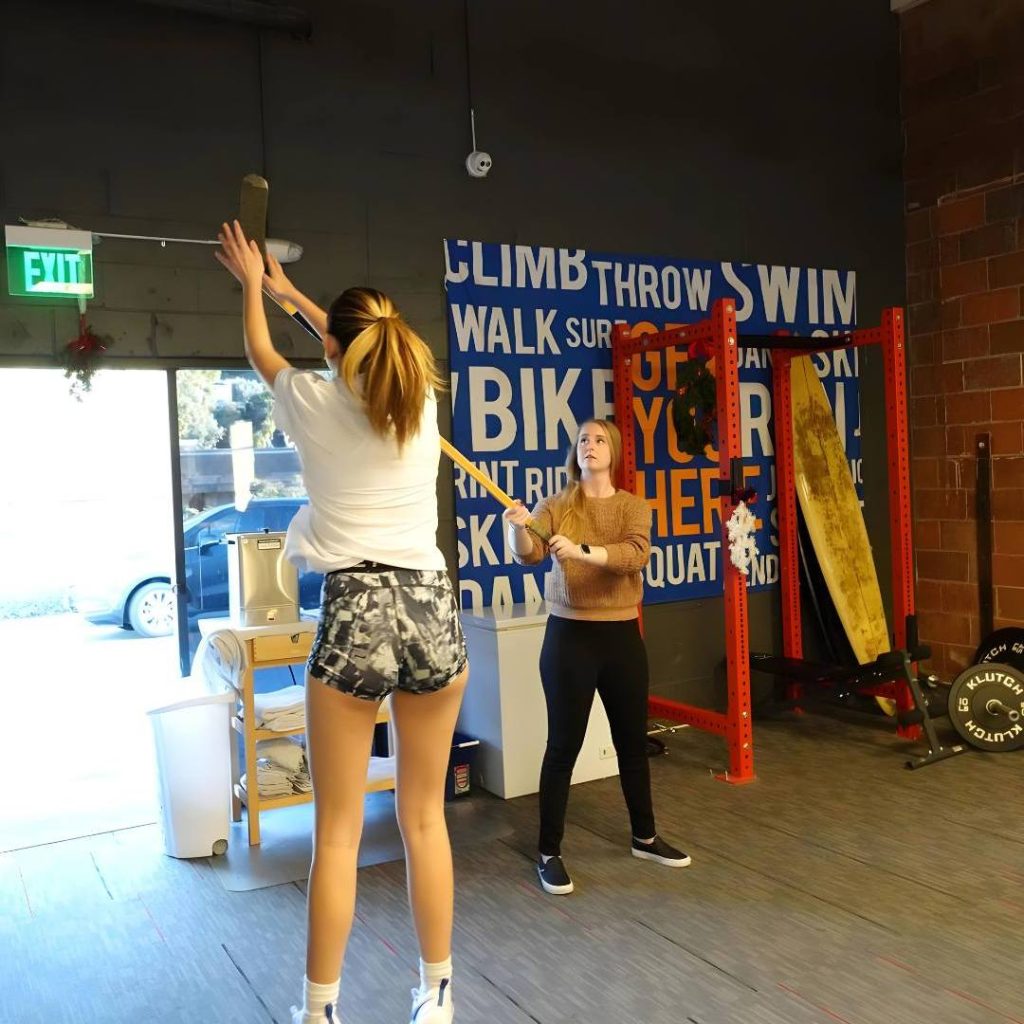 You’ll start to work on making your leg muscles stronger, which takes some of the stress off your knee and cut your pain. Your therapist will give you exercises to do at home and show you how to practice them safely.
You’ll start to work on making your leg muscles stronger, which takes some of the stress off your knee and cut your pain. Your therapist will give you exercises to do at home and show you how to practice them safely. Regain your mobility and rediscover the joy of movement. Our personalized physical therapy programs can help you overcome knee pain and live life to the fullest. Call us today at 949-276-5401. For more tips, follow us on
Regain your mobility and rediscover the joy of movement. Our personalized physical therapy programs can help you overcome knee pain and live life to the fullest. Call us today at 949-276-5401. For more tips, follow us on 



 Train smarter, not harder! Schedule a PT consultation to prevent injuries and reach your running goals. Call us today at 949-276-5401. For more tips, follow us on
Train smarter, not harder! Schedule a PT consultation to prevent injuries and reach your running goals. Call us today at 949-276-5401. For more tips, follow us on 




